WARNING: RISK ASSOCIATED WITH INTRATHECAL USE and NEPHROGENIC SYSTEMIC FIBROSIS (NSF)
Risk Associated with Intrathecal Use
Intrathecal administration of gadolinium-based contrast agents (GBCAs) can cause serious adverse reactions including death, coma, encephalopathy, and seizures. Clariscan is not approved for intrathecal use.
Nephrogenic Systemic Fibrosis
GBCAs increase the risk for NSF among patients with impaired elimination of the drugs. Avoid use of Clariscan in these patients unless the diagnostic information is essential and not available with noncontrasted MRI or other modalities. NSF may result in fatal or debilitating fibrosis affecting the skin, muscle and internal organs.
The risk for NSF appears highest among patients with:
- Chronic, severe kidney disease (GFR < 30 mL/min/1.73m²), or
- Acute kidney injury.
Screen patients for acute kidney injury and other conditions that may reduce renal function. For patients at risk for chronically reduced renal function (e.g., age > 60 years, hypertension, diabetes), estimate the glomerular filtration rate (GFR) through laboratory testing. For patients at highest risk for NSF, do not exceed the recommended Clariscan dose and allow a sufficient period of time for elimination of the drug from the body prior to any re-administration.
PRODUCT INDICATIONS AND USE:
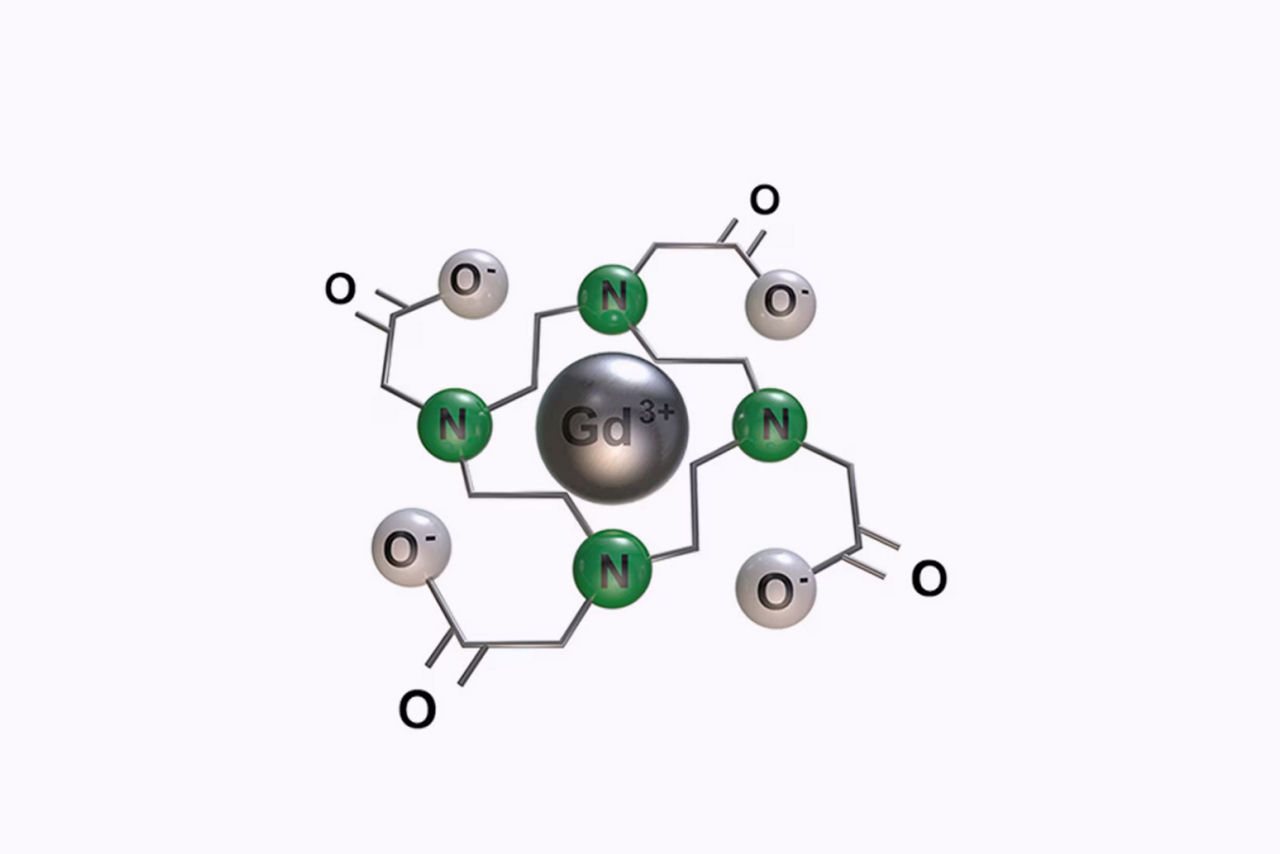
Clariscan™ (gadoterate meglumine) is a prescription gadolinium-based contrast agent indicated for intravenous use with magnetic resonance imaging (MRI) in brain (intracranial), spine and associated tissues in adult and pediatric patients (including term neonates) to detect and visualize areas with disruption of the blood brain barrier (BBB) and/or abnormal vascularity.
CONTRAINDICATIONS
History of clinically important hypersensitivity reactions to Clariscan.
WARNINGS AND PRECAUTIONS
- Risk Associated with Intrathecal Use: Intrathecal administration of GBCAs can cause serious adverse reactions including death, coma, encephalopathy, and seizures. The safety and effectiveness of Clariscan have not been established with intrathecal use. Clariscan is not approved for intrathecal use.
- Nephrogenic Systemic Fibrosis: GBCAs increase the risk for NSF among patients with impaired elimination of the drugs. Avoid use of Clariscan among these patients unless the diagnostic information is essential and not available with non-contrast MRI or other modalities.
- Hypersensitivity Reactions: Anaphylactic and anaphylactoid reactions have been reported with Clariscan, involving cardiovascular, respiratory, and/or cutaneous manifestations. Some patients experienced circulatory collapse and died.
- Before Clariscan administration, assess all patients for any history of a reaction to contrast media, bronchial asthma and/or allergic disorders. These patients may have an increased risk for a hypersensitivity reaction to Clariscan.
- Gadolinium Retention: Gadolinium is retained for months or years in several organs. The highest concentrations have been identified in the bone, followed by other organs (e.g. brain, skin, kidney, liver and spleen). While clinical consequences of gadolinium retention have not been established in patients with normal renal function, certain patients might be at higher risk. These include patients requiring multiple lifetime doses, pregnant and pediatric patients, and patients with inflammatory conditions Minimize repetitive GBCA imaging studies, particularly closely spaced studies when possible.
- Acute Kidney Injury: In patients with chronically reduced renal function, acute kidney injury requiring dialysis has occurred with the use of GBCAs. The risk of acute kidney injury may increase with increasing dose of the contrast agent; administer the lowest dose necessary for adequate imaging
- Extravasation and Injection Site Reactions: Ensure catheter and venous patency before the injection of Clariscan. Extravasation into tissues during Clariscan administration may result in tissue irritation
ADVERSE REACTIONS
- In clinical trials, the most frequent adverse reactions that occurred in > 0.2% of patients who received Clariscan included: nausea, headache, injection site pain, injection site coldness and rash.
- Serious adverse reactions in the postmarketing experience have been reported with Clariscan. Serious adverse reactions include but are not limited to arrhythmia, cardiac arrest, respiratory arrest, pharyngeal edema, laryngospasm, bronchospasm, coma, convulsion, and acute pancreatitis with onset within 48 hours post GBCA administration.
USE IN SPECIFIC POPULATIONS
- Pregnancy: GBCAs cross the human placenta and result in fetal exposure and gadolinium retention. Use only if imaging is essential during pregnancy and cannot be delayed
- Lactation: There are no data on the presence of gadoterate in human milk, the effects on the breastfed infant, or the effects on milk production. However, published lactation data on other GBCAs indicate that 0.01 to 0.04% of the maternal gadolinium dose is present in breast milk.
- Pediatric Use:The safety of Clariscan has not been established in preterm neonates. No dosage adjustment according to age is necessary in pediatric patients.
- Geriatric Use: The use of Clariscan in elderly patients should be cautious, reflecting the greater frequency of impaired renal function and concomitant disease or other drug therapy. No age-related dosage adjustment is necessary.
- Renal Impairment: No Clariscan dosage adjustment is recommended for patients with renal impairment.
To report SUSPECTED ADVERSE REACTIONS, contact GE HealthCare at 1-800-654-0118 or by email at gpv.drugsafety@gehealthcare.com or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
Please see CLARISCAN full Prescribing Information, including the Medication Guide, for additional important safety information.