Don't have an account?
Prevention of Chemotherapy-Induced Cardiotoxicity: The Role of the ECG
By Dr. Payal Kohli, MD, FACC
The field of oncology is exploding. The past few decades have witnessed a surge of targeted chemotherapeutic agents, including immunotherapy agents, which employ the immune system to treat a variety of solid and liquid tumors. Just like everything else in life, however, sometimes fixing one problem can exacerbate another. Cardiologists must find ways to support oncologists, given the advent of many of these new oncological agents run the risk of cardiotoxicity.
From this conundrum of fighting the cancer but hurting the heart, the field of cardio-oncology was born. As one of the most rapidly expanding fields in medicine, it hopes to address, in a multidisciplinary fashion, the effects of cancer and its treatments on the heart, including ways to minimize cardiac toxicity and collateral damage. Cardiotoxicity can take the form of dysfunction with the "pump" (heart failure), dysfunction with the "electricity" (arrhythmias), or even complications with the "plumbing" (ischemic complications or angina).
The Electrocardiogram as a Bedside Tool to Guide Cancer Treatment
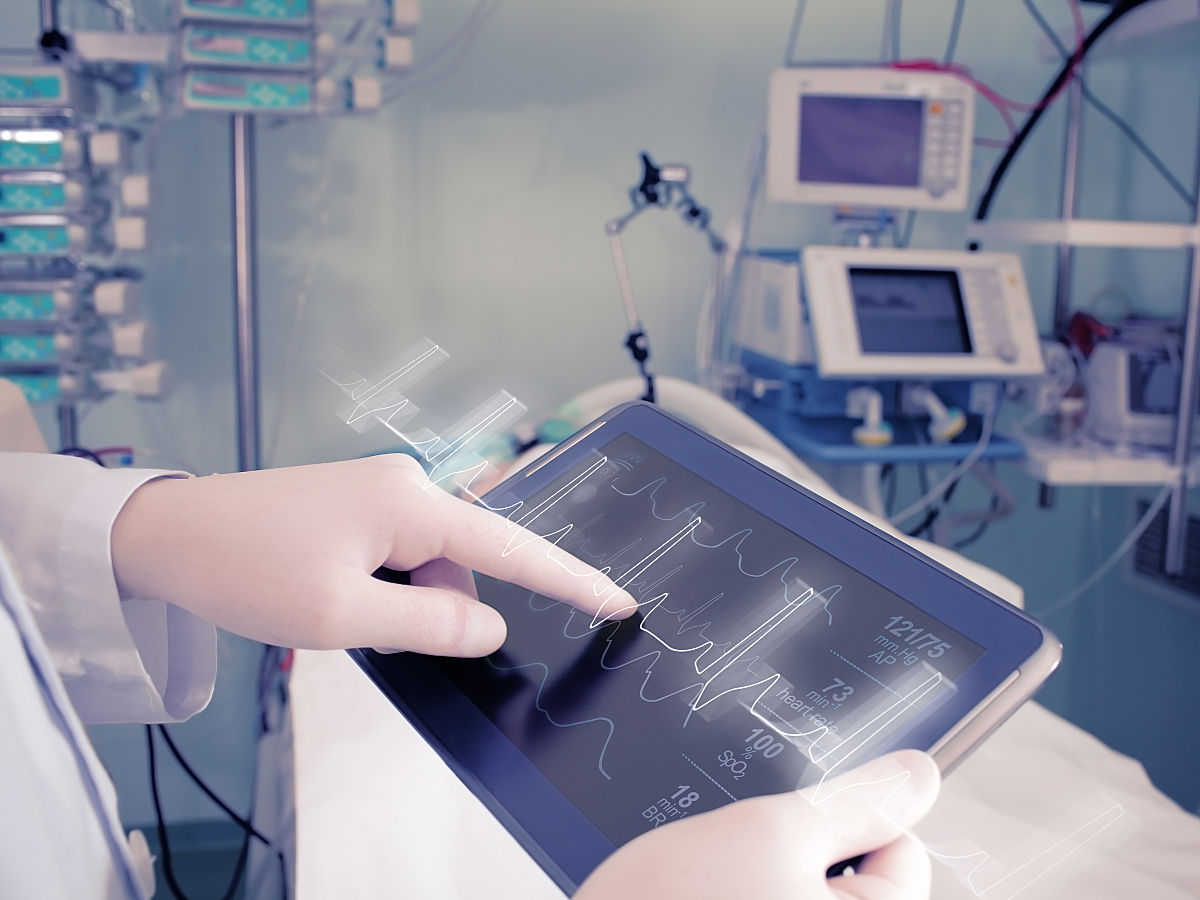
A number of clinical tools monitor for cardiotoxicity, including the echocardiogram, biomarkers, cardiac MRI, and even coronary angiography. However, the electrocardiogram, one of the most fundamental diagnostic tools in a clinician's toolbox, plays a key role in the diagnosis, treatment, and prevention of chemotherapy-induced cardiotoxicity, especially when it comes to problems with the "electricity" or the "plumbing." It is also one of the easiest and most readily available tools at the bedside for clinical diagnosis and serial monitoring. The treating physician must recognize electrocardiographic changes that may herald cardiotoxicity so the dose or frequency of the chemotherapeutic agents may be adjusted or interrupted to minimize or reverse risk of adverse effects on the heart.
Multiple American and European guidelines recommend the use of the standard 12-lead ECG as a critical component of cardiovascular monitoring in patients receiving potentially cardio-toxic chemotherapeutic agents.1, 2, 3 The ECG should be obtained before and during treatment.
Cardiac Risks of Cancer Therapeutics
One of the easily recognized risks of anthracyclines (used in the treatment of breast cancer, sarcoma, leukemia, and lymphomas) and trastuzumab (used for HER2-positive breast cancer) have been left ventricular systolic dysfunction. Not surprisingly, studies have shown those with higher underlying cardiovascular risk (including older age) are more likely to experience cardiotoxicity. This can be due to direct cardiomyocyte damage, change in perfusion of the myocardium, innervation, or the hormonal environment. It can also be due to collateral damage from inflammatory cell infiltration into the myocardium. Radiation therapy also increases cardiovascular risk through some or all of these mechanisms.
However, regardless of the mechanism, the downstream effects of many of these treatments often share the same final pathways with respect to cardiac manifestations of cardiotoxicity, which leads to myocardial dysfunction.
Other conventional chemotherapy agents used in cancer treatment have also been associated with increased risk of cardiac arrhythmias. These include:
- Alkylating agents such as cyclophosphamide and melphalan
- Microtubule-binding agents such as paclitaxel
- Immunomodulatory drugs such as thalidomide
- Targeted agents such as mTOR inhibitors, HER2 inhibitors, BTK inhibitors, BRAF inhibitors, and immunotherapy (immune checkpoint inhibitors and CAR-T cell therapy)
Pro-Arrhythmic Effects of Chemotherapeutic Agents
Studies have shown multiple possible mechanisms of pro-arrhythmic effects of cancer therapeutics.4 Through their effects on cardiac hemodynamics and filling pressures, these agents can lead to atrial and ventricular remodeling and dilation, which can cause effects on the cardiac conduction system and increase risk of both atrial and ventricular arrhythmias. Small vessel coronary ischemia (microvascular spasm) can create micro re-entrant circuits around areas of myocardial scar. Changes in action potential through ion channels can lead to QT prolongation and increase the risk of polymorphic ventricular tachycardia (torsade de pointes). Electrolyte abnormalities as a result of dehydration, vomiting, or diarrhea could also affect electrical conduction and exacerbate or create arrhythmias. Finally, some of these agents can also affect the His-Purkinje system directly.
Electrocardiographic Changes and Impact on Chemotherapy Regimen
Just as elevations in biomarkers such as natriuretic peptides can herald subclinical manifestations of cardiotoxicity (i.e., changes in the filling pressures before cardiac dysfunction has ensued), changes in the ECG can herald subclinical arrhythmias. As an example, excess premature atrial contractions could serve as a warning for impeding atrial fibrillation or excess premature ventricular contractions may precede ventricular arrhythmias, such as non-sustained ventricular tachycardia. These may prompt the clinician to adjust or interrupt the chemotherapy.
Sometimes, the presence of multiple atrial ectopic beats may require stopping chemotherapy in order to prevent atrial fibrillation; the presence of numerous PVCs with multiple morphologies could require discontinuation of chemotherapy due to an increased risk of malignant ventricular arrhythmias, such as polymorphic ventricular tachycardia or ventricular fibrillation.
Similarly, a prolongation of the QT interval can necessitate dose interruption or modification, not just of the chemotherapeutic agent but also potentially other medications (i.e., antibiotics) the patient may be receiving that can affect QTc as part of the comprehensive treatment regimen.
Bradyarrhythmias like sinus bradycardia can present in a more indolent fashion and can easily be missed, especially in the setting of the chronically fatigued cancer patient. However, it is established that taxanes and angiogenesis inhibitors (such as thalidomide) can directly affect the sinus node or other levels of the atrioventricular conduction system, including the infra-hisian system through modulation of the parasympathetic nervous system and create right or left bundle branch block. These effects appear acutely, within hours of starting infusion therapy and can resolve in one to two days of cessation of treatment.5 Some of these agents can also affect conduction indirectly through effects on metabolism or through dysregulation of thyroid homeostasis.6
A Practical Approach to Cardiovascular Monitoring for Cancer Patients
A cardio-oncology expert panel from the French Working Group of Cardio-Oncology has synthesized and consolidated the American and European guidelines to offer a practical approach to the cardiovascular monitoring of the cancer patient.3
The first step is to identify the patient who may be at high risk for the development of cardiac complications of cancer treatment, which includes the older patient, someone with preexisting cardiovascular disease, or one for whom the heart is included in the radiation field (if the patient is receiving chest radiation). Second, a multidisciplinary discussion and ongoing communication between the cardiologist, medical oncologist, and radiation oncologist is critical to ensure successful treatment and monitoring. Third, it is essential to individualize the treatment plan based on the chemotherapeutic regimen being considered. A vital component of this monitoring will include the electrocardiogram, a readily available bedside tool that can have dramatic impacts on the patient's clinical outcomes and can subvert adverse effects before they occur.
Resources
- Beavers CJ, Rodgers JE, Bagnola AJ, et al. Cardio-oncology drug interactions: A scientific statement from the American Heart Association. Circulation. 2022;145:e811–e838. https://doi.org/10.1161/cir.0000000000001056.
- Lyon A, Lopez-Fernandez T, Couch L, et al. 2022 ESC guidelines on cardio-oncology developed in collaboration with the European Hematology Association (EHA), the European Society for Therapeutic Radiology and Oncology (ESTRO) and the International Cardio-Oncology Society (IC-OS). European Heart Journal. 2022;43(41):4229–4361. https://doi.org/10.1093/eurheartj/ehac244.
- Alexandre J, Cautela J, Ederhy S, et al. Cardiovascular toxicity related to cancer treatment: A pragmatic approach to the American and European cardio‐oncology guidelines. Journal of the American Heart Association. 2020;9:e018403. https://doi.org/10.1161/jaha.120.018403.
- Spînu Ș, Cismaru G, Boarescu PM, et al. ECG markers of cardiovascular toxicity in adult and pediatric cancer treatment. Dis Markers. 2021;2021:6653971. doi:10.1155/2021/6653971.
- Rowinsky EK, Eisenhauer EA, Chaudhry V, et al. Clinical toxicities encountered with paclitaxel (Taxol). Seminars in Oncology. 1993 Aug;20(4 Suppl 3):1-15. PMID: 8102012.
- Fahdi IE, Gaddam V, Saucedo JF, et al. Bradycardia during therapy for multiple myeloma with thalidomide. The American Journal of Cardiology. 2004; 93,(8): 1052–55. https://doi.org/10.1016/j.amjcard.2003.12.061.
Dr. Payal Kohli, MD, FACC is a top graduate of MIT and Harvard Medical School (magna cum laude) and, as a practicing noninvasive cardiologist, is the managing partner of Cherry Creek Heart in Denver, Colorado.
The opinions, beliefs, and viewpoints expressed in this article are solely those of the author and do not necessarily reflect the opinions, beliefs, and viewpoints of GE Healthcare. The author is a paid consultant for GE Healthcare and was compensated for creation of this article.
