Don't have an account?
Musculoskeletal Ultrasound: Challenges, Benefits, and Best Practices
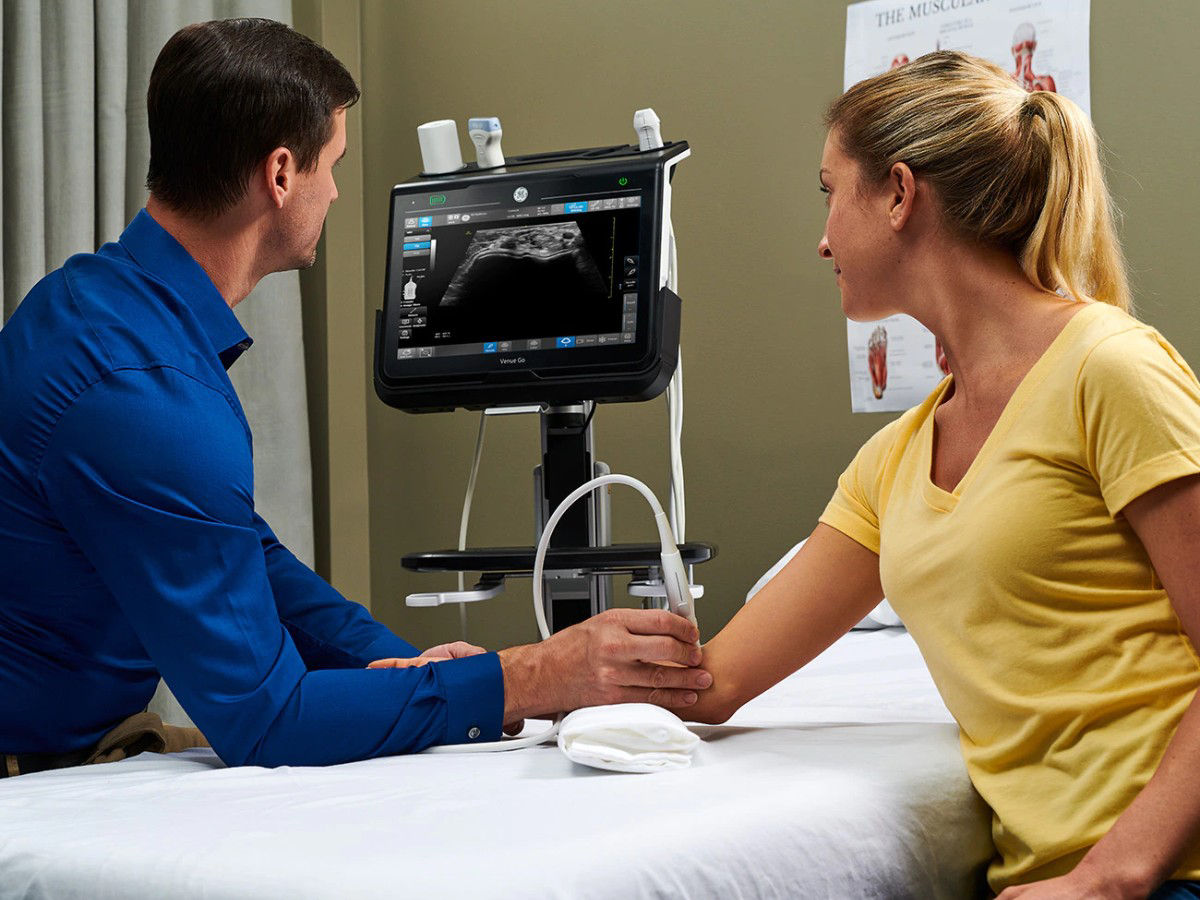
Point of Care Ultrasound (POCUS) has been widely adopted in clinical care in the musculoskeletal setting. In recent years POCUS has provided bedside confirmation of various conditions, giving physicians a range of benefits that lead to better decision-making for improved patient outcomes:
Ease of use. Thorough tutorials and educational resources are available to train physicians on how to use POCUS, providing a convenient option to help clinicians to gain competency quickly.
The applicability of POCUS has become increasingly beneficial for patients with MSK issues affecting the muscles, tendons, ligaments, nerves, and soft tissues.1
Benefits of MSK Ultrasound
A paper in the Journal of Intensive Care shows that in the MSK ultrasound arena, these portable devices can be especially helpful in rapidly identifying soft tissue infections, joint effusions, foreign bodies, long-bone fractures, muscle and tendon injuries, and vascular occlusions.2 POCUS is also showing potential for assessing MSK outcomes in people with hemophilia, according to a paper in Research and Practice in Thrombosis and Haemostasis.3
For pediatric patients specifically, a paper in Children demonstrates the advantages of MSK ultrasound for diagnosing tenosynovitis in juvenile idiopathic arthritis presenting with ankle swelling.4
MSK ultrasound use has also grown exponentially in recent years. For example, a paper in the Journal of the American College of Radiology showed a 347% jump in total MSK ultrasound volume for the evaluation of nonspine joint disease between 2003 and 2015.5 Also, nonradiologists — especially podiatrists in private offices — have shown a growing predilection for this imaging modality.6
Just Below the Surface
With evolving technology, data has shown improved accuracy with POCUS in the MSK setting. Images can be clearly and easily captured, whether to identify more superficial issues located just under the skin or to review multiple layers of muscle and fascia. Specifically, for diagnosing complete rotator cuff tears, for instance, POCUS can be as accurate as MRI.1 It should be noted that MRI remains the gold standard for imaging modality for a wide range of musculoskeletal disorders, but POCUS can be effective at determining if a patient requires an MRI.
As far as who can perform MSK ultrasound, its use is not limited to emergency physicians. Depending on the practice setting, radiologists often can and do take the lead in using POCUS and managing those around them, but many other specialties also benefit including rheumatology, sports medicine, orthopedics, and physiotherapy. Anyone who wants to leverage this technology to more efficiently use their time can do so. The key is proper training.
Training Opportunities
While many clinicians learn ultrasound skills through their own clinical experience, several organizations including the Society of Hospital Medicine and the American College of Physicians offer broad POCUS training, both virtually and in person. 7,8 Additional musculoskeletal components for those interested in incorporating it into their practice can also be found through in-person courses geared specifically to orthopedics. Device manufacturers even offer a wide variety of educational resources for practitioners preferring to learn on their own.
The training is not just for physicians but for other healthcare professionals as well whose training should be ongoing. A research report in Anatomical Sciences Education showed that medical students learning MSK ultrasound gained confidence in their clinical and anatomical skills, making it a multifaceted tool.9
Proper training for POCUS typically requires the comprehension of ultrasound physics, machine modes, and image orientation as well as obtaining quality and accurate images. Becoming proficient in MSK ultrasound also specifically necessitates knowledge of commonly seen pathologies in addition to recognizing when another imaging modality would be proper to obtain a diagnosis. Additionally, MSK ultrasound practitioners need to make sure their knowledge of anatomy in areas like the shoulder, knee, and ankle is proficient enough to be able to recognize the variations in appearance on imaging.
Practical Lessons
Logistical lessons also need to be learned when becoming proficient in POCUS. For example, most devices allow images to be stored on the device, but users should download these to a picture archive and communication system (PACS). Each hospital or healthcare system might have a different workflow, but for the system to work optimally, all patient ultrasound examinations should be formally documented in permanent medical records with easily retrievable images. This not only saves time down the line but also allows for the comparison of images in the future.
Although MSK POCUS is not an invasive procedure, the probes and nonsterile gel can spread infection if contaminated. One study published in Clinical Orthopaedics and Related Research found increased risk of contamination following simulated intraarticular injections of the shoulder when ultrasound probes and transmission gel were used.10 Best practices would suggest that users should adhere to strict infection prevention and control measures to prevent contamination.
MSK ultrasound is an important complementary—and in some cases alternative—technique to help tailor more efficient patient care. It helps physicians identify a range of musculoskeletal conditions such as joint effusions, muscle and tendon injuries, and soft tissue issues, among others. Using POCUS within the MSK care area gives physicians the tools needed for faster decision-making to help patients move toward healing and improved health.
References:
- Arnold MJ, Jonas CE. Point-of-care ultrasonography. American Family Physician. 2020 Mar;101(5):275-285. https://pubmed.ncbi.nlm.nih.gov/32109031.
- Chen K-C, Lin A C-M, Chong C-F, et al. An overview of point-of-care ultrasound for soft tissue and musculoskeletal applications in the emergency department. Journal of Intensive Care. 2016;4(55). https://jintensivecare.biomedcentral.com/articles/10.1186/s40560-016-0173-0.
- Bakeer N, Dover S, Babyn P, et al. Musculoskeletal ultrasound in hemophilia: Results and recommendations from a global survey and consensus meeting. Research and Practice in Thrombosis and Haemostasis. 2021;5(5):e12531. https://onlinelibrary.wiley.com/doi/10.1002/rth2.12531.
- Paolera SD, Pastore S, Zabotti A, et al. Ultrasonographic assessment for tenosynovitis in juvenile idiopathic arthritis with ankle involvement: diagnostic and therapeutic significance. Children. 2022;9(4):509. https://www.mdpi.com/2227-9067/9/4/509.
- Kanesa-thasan RM, Nazarian LN, Parker L, et al. Comparative trends in utilization of MRI and ultrasound to evaluate nonspine joint disease 2003 to 2015. Journal of American Colleg of Radiology. 2018;15(3 Pt A):402-407. https://www.jacr.org/article/S1546-1440(17)31300-5/fulltext.
- Sharpe RE, Nazarian LN, Parker L, et al. Dramatically increased musculoskeletal ultrasound utilization from 2000 to 2009, especially by podiatrists in private offices. Journal of American Colleg of Radiology. 2012;9(2):141-146. https://www.jacr.org/article/S1546-1440(11)00522-9/fulltext.
- POCUS Certificate of Completion. Society of Hospital Medicine. https://www.hospitalmedicine.org/clinical-topics/ultrasound/pocus-certificate-of-completion/. Accessed April 20, 2022.
- Point of Care Ultrasound (POCUS) for Internal Medicine. American College of Physicians. https://www.acponline.org/meetings-courses/focused-topics/point-of-care-ultrasound-pocus-for-internal-medicine. Accessed April 20, 2022.
- Brown CC, Arrington SD, Olson JF, et al. Musculoskeletal ultrasound training encourages self-directed learning and increases confidence for clinical and anatomical appreciation of first-year medical students. Anatomical Sciences Education. 2021;Epub ahead of print. https://anatomypubs.onlinelibrary.wiley.com/doi/10.1002/ase.2145.
- Sherman T, Ferguson J, Davis W, et al. Does the use of ultrasound affect contamination of musculoskeletal injections sites? Clinical Orthopaedics and Related Research. 2015;473(1):351-357. https://journals.lww.com/clinorthop/Fulltext/2015/01000/Does_the_Use_of_Ultrasound_Affect_Contamination_of.63.aspx.
