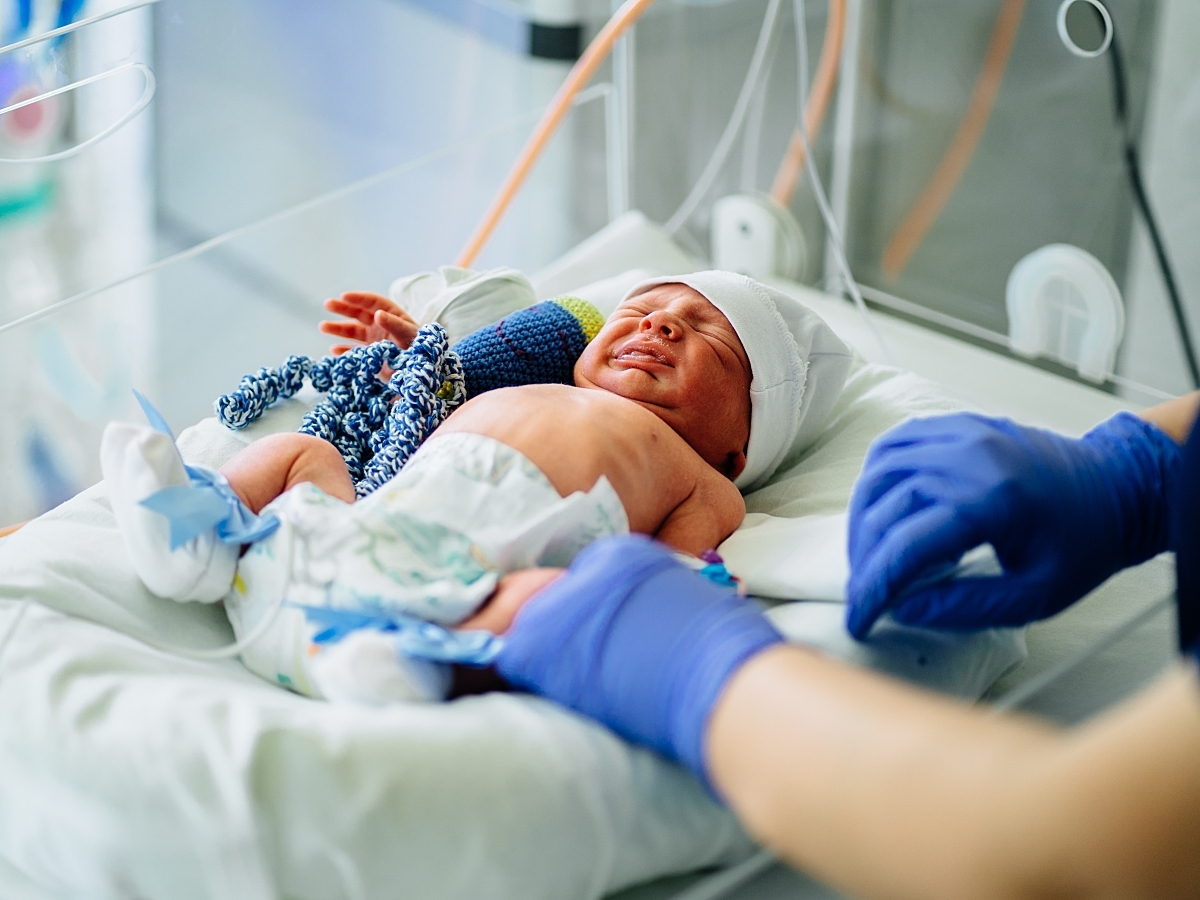
From the moment of birth, temperature regulation is critical for all newborns—especially those born prematurely. Improvements in newborn mortality were first linked to care in an incubator in a historic study published in 1958 in Pediatrics.1 Since that time, other studies and clinical observations have found that hypothermia (defined as a body temperature less than 36.5°C) and hyperthermia (defined as a body temperature above 37.5°C) are both detrimental to a newborn's health.
In spite of modern technology, NICU temperature regulation can be challenging. Quality improvement efforts to manage preterm and term infant admission temperatures have proven effective, according to research published in the Journal for Specialists in Pediatric Nursing.2 Ongoing training of staff is critical to success.
Best Practices for NICU Temperature Regulation
Although dealing with admission temperatures can be challenging for many reasons, ongoing NICU temperature regulation requires attention and expertise. Using an incubator bed that regulates an infant's temperature through a computer algorithm based on the temperature measured by a skin probe—known as servo-control or "baby mode"—does provide more stable infant temperatures, but it also requires more and different expertise from the nurse. Several practices can influence this for better or worse. Here are some best practices for ongoing NICU temperature regulation.
Preheating
Do not place the temperature probe under the warmer while preheating. This serves to warm the probe before it is attached to the infant and may lead to a falsely high temperature reading. This could delay the appropriate output of heat, risking hypothermia.
Probe Placement
The probe must remain in full contact with the infant's skin and be covered by a reflective patch. The reflective patch serves to reflect the heat so that it is not directly focused on the probe, which also helps prevent inaccurately high readings.
The probe should be placed so that the infant does not lay on it. Placing a probe under the infant's body can result in "insulation" of the probe and a higher temperature reading. This, again, will result in lower heat output and the potential for hypothermia.
Various studies have looked at probe placement, but most recommendations come from practice guidelines and manufacturer's recommendations, according to research published in Advances in Neonatal Care.3 A Cochrane review recommends the abdominal wall as the preferred site for accurate temperature maintenance in servo-control settings.4 A separate Advances in Neonatal Care study of a small sample of 12 preterm infants found axillary and abdominal temperature probe placement to be comparable and effective in maintaining thermoregulation.5 Finally, a third study published in Advances in Neonatal Care found abdominal, flank and axillary skin temperature readings via probe were all comparable and resulted in effective thermoregulation.6
These last two findings conflict with the first Advances in Neonatal care study, which warns against placing the probe in an area of brown fat—abundant later in gestation and located in the axillary area. Axillary placement may be more effective in preterm infants, particularly in very low birth weight infants, as brown fat is unlikely to be present.
All literature agrees with avoiding bony prominences that can result in skin breakdown and avoiding placing the probe underneath the infant. For this reason, many nurses prefer to use axillary placement, seeing as the infant can be turned from prone to supine without moving the temperature probe. Others suggest placing two skin probes: one on the abdomen and one on the flank. Using a probe that plugs into the incubator bed helps avoid moving the infant too frequently.
Probe Management
Nurses should ensure that the incubator bed is changed to "air mode" when the probe is removed for routine replacement or for other tasks, such as bathing the infant. A bed left in baby mode will respond to the removal of the probe by increasing heat output.
Infants are often held with the probe still attached for temperature monitoring. In this case, the bed should be in air mode prior to removing the infant. This allows the bed to maintain the air temperature at the point that the infant was previously experiencing. If it's in baby mode, the bed will continue to heat based on the infant's temperature while they are being held.
Maintaining a Neutral-Thermal Environment
A neutral-thermal environment (NTE) refers to the range of air temperature in which the infant's body temperature is maintained. To create the ideal NTE, their temperature must hold steady within a normal range without an increase in metabolic demand and increased need for oxygen and/or glucose.
The ideal temperature range isn't the same for all newborns. Factors to consider when calculating NTE include:
- Gestational age
- Birth weight
- Chronologic age
- Humidity
- Use of positioning devices
- Any clothing or swaddling
Gestational age and day of life are the two critical data points that are needed to determine a starting temperature. However, if an NTE has already been established and an infant is being transitioned, such as moving from one bed to another, the established temperature should be used.
The calculated NTE is a good place to start when pre-heating the bed. Once the infant is placed in the bed and the bed is on baby mode with a temperature probe in place, the ideal environmental temperature is ensured. It is important to ensure that a bed is not overheated while awaiting admission or during other activities. Beds are very efficient at warming, but cannot cool an infant.
Navigating Temperature Variability
Axillary temperature measurement is the most common method employed in the NICU. However, there are several things that can impact the accuracy of these temperature readings, including infant position (measurement in the axilla that the infant is laying on, measurement in the axilla if the infant is laying with an arm over the head), presence of bundling/swaddling and variability in instruments used for temperature measurement. It's important to consider not only temperature measurements at a single point in time but also temperature trends.
This is particularly important when caring for an infant in a Giraffe OmniBed in baby mode. The skin temperature probe readings should be documented, along with environmental temperature and the baby's reference temperature, at predetermined time points, usually every three to six hours. When the bed is receiving accurate data from the temperature probe, it is capable of maintaining the infant's body temperature within the desired range.
If the infant needs more support to maintain temperature, with a stable body and skin temperature but rising environmental temperature, it may point to an infection or other abnormality. Watching temperature trends over time can provide valuable information in the care of sick and premature infants.
It is important to note that skin and axillary temperatures may not match. The evaluation of trends helps to evaluate changes. For instance, taking the axillary temperature and recording the skin temperature over two to three episodes may reveal a difference of 0.5 degrees or greater. This difference is usually consistent and can be used to watch without disturbing the infant frequently to measure axillary temperature. This correlation should be measured whenever the temperature probe is moved to a new location, as the degree of difference will likely change.
Instruments used to measure actual body temperature via any route, whether axillary, tympanic or temporal, often use a predictive algorithm. This predictive algorithm allows for a shorter duration of actual contact. Based on the temperature rise during a few seconds of contact, the actual temperature is predicted. This means there is variability in how the temperature reading would compare to a mercury-in-glass thermometer. The range within which the temperature is measured meets valid criteria, but temperature measures outside an expected range should be validated by repeating the measurement as well as watching temperature trends over time.
The Giraffe OmniBed has two different types of heat algorithms that are both deployed when there is a deviation of +/- 0.5 degrees C from the set point. These are referred to as the cascade control or proportional control algorithms. The cascade control algorithm is used to maintain the infant's temperature more gradually in an effort to avoid overshooting the control point. The proportional control algorithm provides more or less heat to maintain the infant's temperature at the desired point. If the temperature is rising or falling quickly, heat is regulated accordingly.
Transitioning to Air Control
The trend screen on the bed display provides a useful reference of all temperature data points, including favorable temperature ranges where stable infant temperatures are detected. This information can help determine the ideal environmental temperature range and can help inform whether an infant is ready to transition to air control, as well as what air temperature would be appropriate during the transition.
Modern technology provides infant care staff with the tools they need to accomplish NICU temperature regulation. Following best practices for probe management and temperature recording can help support the best possible outcomes for the infants in your care.
References:
- Silverman W, Fertig J, Berger A. The influence of the thermal environment upon the survival of newly born premature infants. Pediatrics. November 1958; 22 (5): 876–886. doi:10.1542/peds.22.5.876
- Donnellan D, Moore Z, Patton D, O'Connor T, Nugent L. The effect of thermoregulation quality improvement initiatives on the admission temperature of premature/very low birth‐weight infants in neonatal intensive care units: A systematic review. Journal for Specialists in Pediatric Nursing. 2020;25(2). doi:10.1111/jspn.12286
- Joseph RA, Derstine S, Killian M. Ideal site for skin temperature probe placement on infants in the NICU. Advances in Neonatal Care. 2017;17(2):114-122. doi:10.1097/anc.0000000000000369
- Sinclair J. Servo‐control for maintaining abdominal skin temperature at 36C in low birth weight infants. Cochrane Database of Systematic Reviews. doi.org/10.1002/14651858.CD001074
- National Association of Neonatal Nurses. Research abstracts from the 2016 NANN Research Summit. Advances in Neonatal Care. 2016;16(3):E3-E12. doi:10.1097/anc.0000000000000287
- Schafer D, Boogaart S, Johnson L, et al. Comparison of neonatal skin sensor temperatures with axillary temperature. Advances in Neonatal Care. 2014;14(1):52-60. doi:10.1097/anc.0000000000000027